NOTE: I am not a medical expert. In this blog post, my goal is to share with you my own experiences and those of my family, along with research I have done. As always, check with your doctor before trying anything new.
Shortly after writing my recent post on My Experiences with COVID and ME/CFS, I realized I had left out some of the most important information: what I had done (and what treatments are available) to treat COVID and prevent side effects, severe COVID, or a worsening of my ME/CFS. So, that's what this post will cover.
To clarify, this post is relevant for:
- Anyone who has ME/CFS or long COVID (which is usually ME/CFS)
- Anyone, even without underlying medical conditions, who gets COVID
- Anyone who had COVID and is suffering from lingering symptoms, i.e. long COVID
With ME/CFS, Prepare Before You Get COVID
If you have ME/CFS, I'm sure you're aware by now that COVID presents some serious possible effects, beyond those in the general population. Our immune systems don't work normally and we don't fight infections the way we should. Also, as anyone with ME/CFS has probably experienced, just being exposed to even a mild infection, like a cold, can often trigger a long-term worsening of all of our usual symptoms (this is because our immune systems are over-reacting, even after the infection clears up).
COVID, however, is proving to be an even stronger trigger than most infections. In studies, for most common infections that can trigger ME/CFS to start--like mono/glandular fever, parvovirus, Lyme disease, and others--about 10% of those who get infected do not recover but go on to develop ME/CFS. So far, studies show that between 30-50% of those who get COVID do not fully recover but develop lingering symptoms (that are often ME/CFS). Those numbers are stunning! This failure to recover after the infection clears is what is being called "long COVID" in the media.
So, if you already have ME/CFS and then get COVID, your chances of lingering symptoms and/or a long-term worsening of your underlying disease are quite high.
 |
| Fully vaccinated in June! |
For that reason, it makes sense to do everything possible to avoid getting COVID (for everyone because even a very healthy person could develop long COVID), and especially if you already have ME/CFS. That includes getting vaccinated, if you and your doctor decide it is safe for you to do so. That is an entirely different topic that I have already covered here on the blog. Refer to My Experiences with COVID and ME/CFS for links to my three posts on deciding whether to get the vaccine and how to prepare first. I did get the first two vaccines but later tests showed that I did not make many antibodies. In addition to considering vaccines, wear masks (experts now recommend medical/surgical masks or KN-95's). And, of course, it is still wise to avoid crowds or any groups without masks.
 |
| Double-masked now |
If you have ME/CFS and have not gotten COVID yet, congratulations! Do everything you can now to give yourself a better chance of recovering if you do get it. That includes topics covered in my vaccine prep post, like:
- Improve methylation.
- Treat underlying infections and Normalize your immune system, as much as possible:
- Treat Orthostatic Intolerance (OI).
- Correct sleep dysfunction.
In other words, do as much as you can to improve your overall condition, which will improve your life and reduce the chance of a worsening if you get COVID. This post summarizes all of the treatments that have been effective for my sons and I. Many of these treatments in that post and listed above are inexpensive and readily available. Some can even be tried without a doctor, if you don't have a cooperative doctor willing to help you. I am mostly recovered from COVID, after six weeks, except for slightly reduced energy/stamina that are slowly improving. I believe that all of these treatments I did over the previous years to improve my overall condition with ME/CFS helped me to recover more quickly.
For Anyone: What To Do If You Get COVID
Whether you have ME/CFS or not, there are some simple things you can do at the first signs of COVID infection to prevent serious complications and/or lingering symptoms (long COVID or a worsening of your ME/CFS). There are also some newer treatments that are available, if you can get access to them. Let's start with those.
Approved, Effective Treatments for COVID
There are now two main types of treatments available for COVID that are meant to be used early in the infection at home and to prevent complications and hospitalization:
- Oral COVID Antivirals (Paxlovid and molnupiravir - see article)
- Monoclonal Antibodies
These treatments are intended for use in those at increased risk for severe illness (that would include those with asthma and other lung conditions, older adults, and yes, those with ME/CFS or other immune issues) and are intended to be used to help prevent hospitalizations.
The problem? Since the holiday surge, they have been mostly unavailable. The two new antivirals were released around Christmas-time and were immediately sold out everywhere--too much demand and not enough initial supply. While monoclonal antibodies are not that new, they have also been unavailable for most patients recently, with limited supplies being used for those already in hospitals. My 96-year-old father-in-law is in a nursing home, and he and I both got COVID the first week of January. We could not get either of these treatments for either of us, not even through the nursing home! Hopefully, those supply issues will be worked out, as more is manufactured and infection rates drop in the spring. My primary care doctor said the next shipments of the antivirals are expected in March.
Alternative Treatments
With the official, approved treatments unavailable, some doctors have turned to alternatives. See the NIH page on COVID antiviral treatments for details and talk to your doctor:
- Ivermectin - despite all the media controversy, this antiparasitic drug has shown some effectiveness in limited trials in other countries, but there have been no controlled studies proving its effectiveness. Some doctors are prescribing it, but it is also widely unavailable due to increased demand.
- Fluvoxamine - this SSRI (anti-depressant) showed some effectiveness in limiting serious complications in a study in Brazil. My own doctor prescribed a short course for me for 10 days, when we determined that antivirals and monoclonal antibodies were unavailable.
At-Home Treatments
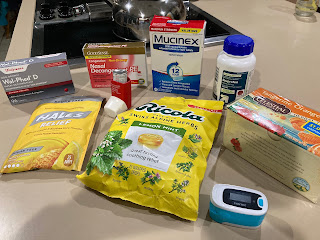
With most cases of COVID, primary symptoms include chest congestion, cough, chest tightness, and sometimes sinus congestion and/or shortness of breath (plus severe fatigue). My son and I both had most of that, except for shortness of breath. You want to prevent those symptoms from becoming severe and doing long-term damage to your lungs and heart. These simple over-the-counter or prescription remedies can help to keep sinuses and lungs clear and ease symptoms:
- Mucinex 12-hour Maximum Strength (1200 mg extended-release guaifenesin) - thins mucus to keep it from collecting in sinuses and lungs and becoming infected - we use it often for allergies and colds, to prevent bronchitis and sinus infection, but we took it round-the-clock (every 12 hours) while we had COVID. Get the kind I linked to above, with no other ingredients in it.
- For sinus congestion, phenylephrine (mild decongestant, sold as Sudafed PE or decongestant PE) or pseudoephedrine (strong decongestant, often sold as Sudafed or decongestant - can't be sold online because you must show ID at the drugstore). Pseudoephedrine can have some side effects, as it constricts blood vessels (which can actually help OI) and is stimulating, so save it for severe congestion. I take PE daily for allergies but only take pseudoephedrine when I get a bad headache (that vaso-constriction makes it very effective for headaches).
- Throat lozenges/cough drops for cough, sore throat, and throat irritation due to cough. I lost my voice during COVID from the constant coughing, and these were very soothing and allowed me to sleep. Be sure they are SUGAR-FREE or they can worsen yeast overgrowth (which many with ME/CFS have) and make you feel worse. I like Hall's Sugar-Free Lemon Honey or Ricola Sugar-Free Lemon Mint herbal drops (my new favorite), but they come in all kinds of flavors.
- Albuterol inhaler (prescription required) for chest tightness, cough, congestion, or shortness of breath - these require a prescription from your doctor but can provide extra relief (and prevention of serious complications) by dilating (opening up) bronchial pathways. I already had one for bronchitis, and I used it a few times at bedtime so that I could fall asleep without having a coughing fit. If breathing in deeply makes you start coughing, you may need an inhaler.
- Ibuprofen or acetaminophen for reducing fever. Ibuprofen will also reduce inflammation. Follow dosing guidelines, especially with acetaminophen, which can damage the liver if you use too much.
- AVOID oral steroids or a steroid inhaler, unless your doctor deems them absolutely necessary and then only use for a short period. Steroids suppress the immune system so are not a good idea when fighting an infection or when you have ME/CFS (in which parts of the immune system are already suppressed). They can be used for short periods to decrease inflammation.
- Get an inexpensive Pulse Oximeter to monitor your blood oxygen saturation level. If it dips below 90%, you should call your doctor and/or go to the emergency room.
- Watch for signs of secondary bacterial infections, like bronchitis or sinus infection, and treat with antibiotics before they get serious. Although my primary care doctor said they are not seeing a lot of secondary bacterial infections with COVID generally, those with ME/CFS tend to be more susceptible to bacterial infections (our dysfunctional immune systems usually over-react to viruses but under-react to bacteria). Bacterial infections need immediate treatment with antibiotics to prevent them from developing into something even worse, like pneumonia. In my case, since I have a long history of bacterial bronchitis, my doctor started me on Zithromax (antibiotic that works against bronchitis) the first day I woke up with chest congestion and called her--not for COVID (it's a virus) but because my congestion was very likely to develop into bronchitis, given my history. If you suspect a secondary infection, like bronchitis or sinus infection, call your doctor immediately.
- Lots and lots of fluids. You can easily get dehydrated when you are sick, which can make everything worse. Plus, lots of fluids--especially hot herbal tea with a touch of honey in it--can soothe a sore throat. My favorites are Celestial Seasonings Zinger herbal teas.
- LISTEN TO YOUR BODY AND REST!! After 20 years with ME/CFS, I thought I knew fatigue, but wow, COVID knocked me out. I mostly slept and ate for 2-3 weeks (and my healthy son was very sick for a week). I am still, six weeks later, needing more sleep at night than usual, have lower energy, and more post-exertional malaise (PEM) than before COVID. All of this is getting better but slowly. Forget about doing anything at all and rest as much as your body needs.
Those are my tips for easing your symptoms when you have COVID and for preventing serious complications or worsening with COVID, based on our own experiences.
What have been YOUR experiences with COVID? What helped you?
Note: This post contains affiliate links. Purchases from these links provide a small commission to me (pennies per purchase), to help offset the time I spend writing for this blog, at no extra cost to you.


No comments:
Post a Comment